Learn the Median and ulnar nerve decompressions surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Median and ulnar nerve decompressions surgical procedure.
Compression of the ulnar nerve within Guyon’s canal is uncommon and is often seen in association with a local space occupying lesion such as an aneurysm or a piso-triquetral ganglion.
Median nerve compression within the carpal tunnel however, represents the commonest peripheral nerve entrapment treated by hand surgeons.
Decompression of each nerve individually is dealt with in the relevant sections on Orthoracle.com
In the rare situation that both median and ulnar nerves are compressed at the wrist, decompression and complete visualisation of both nerves may be achieved through a single ulnar sided approach which is described here.
All of the typical causes of median or ulnar nerve entrapment described elsewhere may contribute to a combined compression.
In the setting of a peripheral nerve clinic, combined compression of both median and ulnar nerves at the wrist is often seen in the context of a more proximal, cord or trunk level brachial plexus injury. Observing such patients recovery over several months may reveal a sudden slowing or even arrest of regeneration as the regenerating front approaches a fibro-osseous canal or tunnel. Although still poorly understood, some authors suggest that this phenomenon relates to an auto-compression of the nerve as it’s volume increases during axonal regeneration.
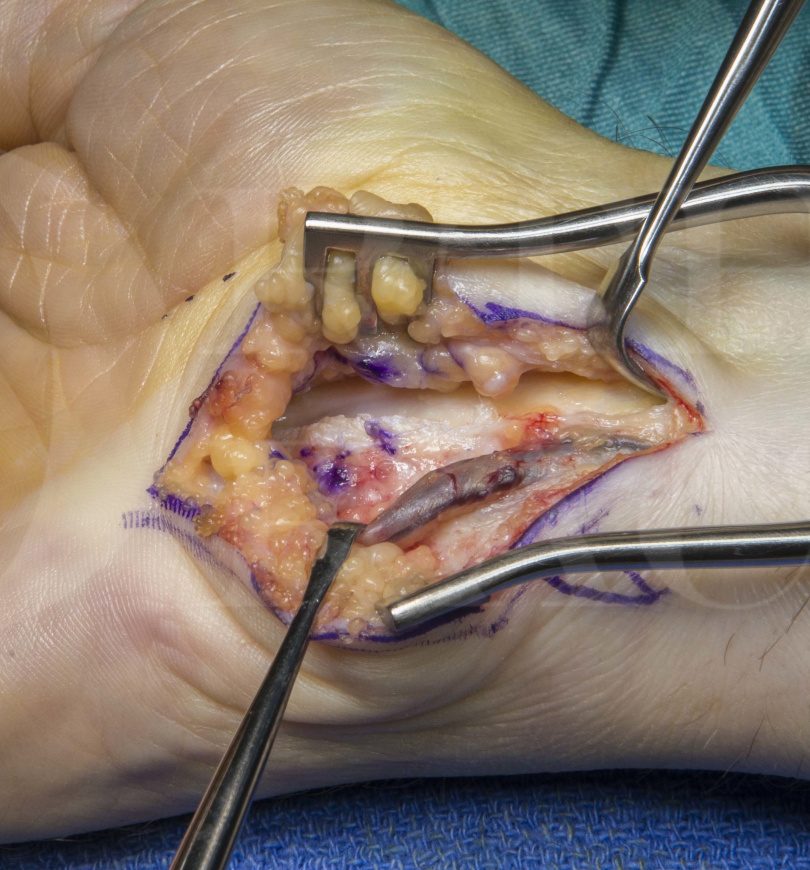
The key factors for a successful outcome in combined median and ulnar nerve decompression through a Guyons canal approach are firstly, adequate decompression and visualisation of the deep motor branch of the ulnar nerve by careful division of the hypothenar tendinous arch at the hook of hamate, and secondly, decompression of the median nerve by release of the transverse carpal ligament from its ulnar sided attachments.
Readers will also find the following associated techniques of interest:
Extended approach Carpal Tunnel decompression
Revision carpal tunnel decompression and application of Polyganics Vivosorb membrane
Carpal tunnel decompression
Median nerve neurolysis, resection and reconstruction using Axogen AVANCE processed nerve allograft

INDICATIONS
Current indications for carpal tunnel decompression are the presence of symptoms for three months or more and failure of non-operative measures such as night splints or steroid injections to provide adequate symptom relief. The presence of sensory or motor axonal loss is an indication for more urgent surgical intervention.
Decompression of the ulnar nerve within Guyon’s canal is performed for local compression due to a local tumour, ganglion, or local trauma to the nerve. It is is an uncommon site of nerve compression. Other less common causes include an pseudoaneurysm, or aneurysm related to hypothenar hammer syndrome. Chronic compression in cyclisting enthusiasts is occasionally seen, as is a non-union of the hook of hamate.
Combined median and ulnar nerve compression at both Guyon’s canal and the carpal tunnel are uncommon. In my peripheral nerve practice, combined compression of both median and ulnar nerves at the wrist often occurs in the context of a more proximal, cord or trunk level brachial plexus injury. Observing such patients recovery over several months may reveal a sudden slowing or even arrest of regeneration as the regenerating front approaches a fibro-osseous canal or tunnel. Although still poorly understood, some authors suggest that this phenomenon relates to an auto-compression of the nerve as it’s volume increases during axonal regeneration.
If simultaneous decompression of both nerves is indication a single approach as detailed here provides complete decompression and direct visualisation.
SYMPTOMS & EXAMINATION
Patients may complain of both ulnar and median sensory symptoms with pain, parasthesia and numbness over all finger tips. Sparing of both the territory supplied by the palmar cutaneous branch of the median nerve (the skin over the thenar eminence) and the dorsal sensory branch of the ulnar nerve (the skin over the dorsum of the 4th and 5th metacarpals) precludes a more proximal compression. Localisation may be further confimed if either compression is severe enough to have lead to motor weakness or muscle wasting. Typically the ulnar sided FDPs would be spared in a Guyons canal entrapment of the ulnar nerve. The ulnar innervated intrisics may be weak and wasted and Froments sign may be positive. (A paper test that demonstrates use of flexor pollicis longus to compensate for a weak adductor pollicis). Similarly, severe median nerve compression at the carpal tunnel may cause thenar muscle wasting. A Tinel-Hoffman sign is useful to locate the site of compression and to rule out more proximal sites of compression. An assessment of radial and ulnar pulses at the wrist and an Allens test is important to assess ulnar artery function and to establish the dominant blood supply to the hand.
INVESTIGATIONS
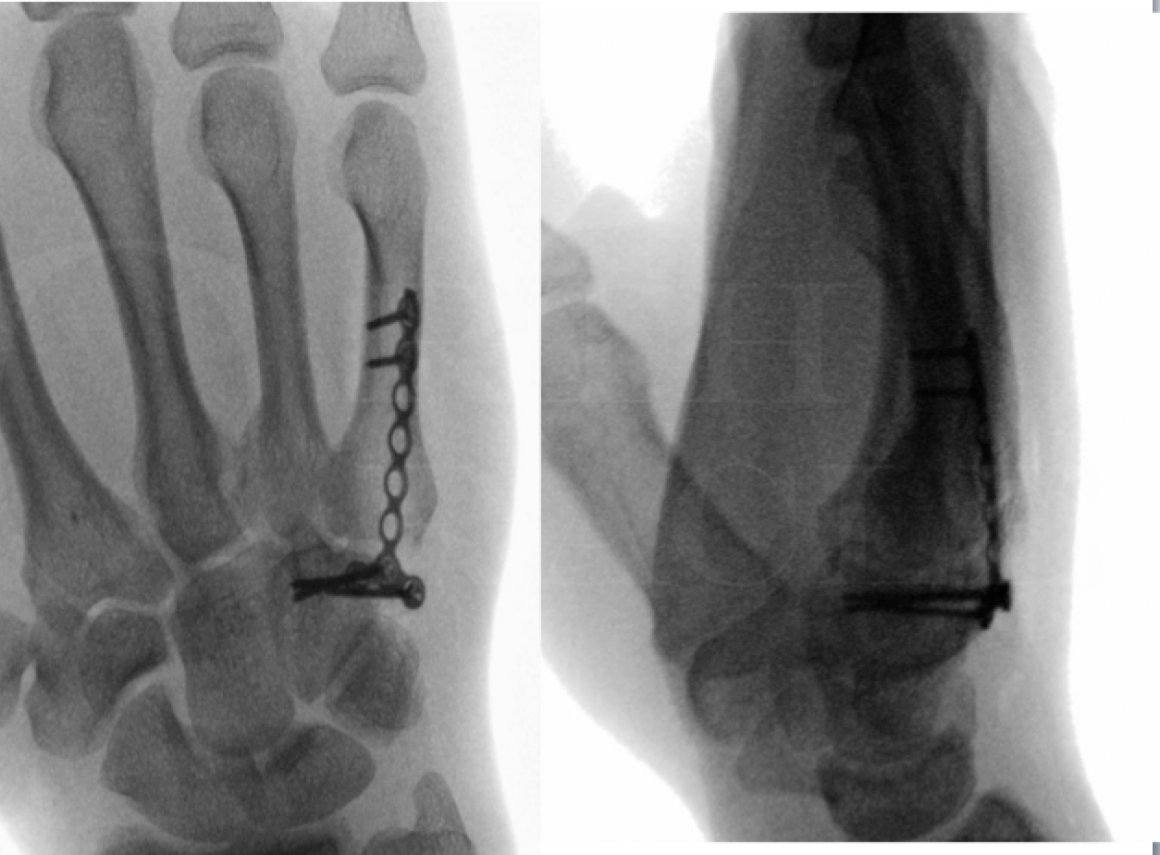
Plain radiographs may demonstrate joint degeneration at the piso-triquetral joint or a non-union of the hamate.
An ultrasound or MRI scan may be useful where compression in Guyons canal is suspected and may demonstrate a space occupying lesion. This is an important part of the investigation.
Median nerve compression at the carpal tunnel does not typically require imaging as a prelude to surgery.
Neurophysiology will demonstrate slowing of conduction velocities across the carpal tunnel and Guyon’s canal. In more significant or prolonged compression ectromyography may demonstrate an element of denervation within the intrinsic muscles. Abductor pollicis brevis (APB) is typically tested in carpal tunnel syndrome and the adductor pollicis or first dorsal interosseous (FDI) for the ulnar nerve. Testing may demonstrate denervation manifested by the presence of positive sharp waves and fibrillations.
ALTERNATIVE OPERATIVE TREATMENT
In severe compression syndromes with longstanding muscle wasting and functional loss, decompression may fail to restore motor function. Consideration must therefore be given to tendon transfers for thumb opposition and anticlaw procedures. These may be performed at the time of nerve transfer if motor recovery is expected to be incomplete.
NON-OPERATIVE MANAGEMENT
Once sensory or motor loss have become established, surgical decompression is mandated and non-operative measures may delay definitive treatment and compromise the final outcome. Early Guyon’s canal entrapment may be successfully treated with splinting. The various non-operative measures for carpal tunnel syndrome and their exact role are detailed in the relevant section.
CONTRAINDICATIONS
Surgical decompression is contraindicated if the patients general fitness precludes surgery. Surgery should be delayed if there is local infection.

Under either general or regional anaesthesia, the patient is positioned supine with the arm on an arm table.
An upper arm tourniquet is applied.
The hand is placed into a lead hand.
Loupe magnification is essential.
Bipolar diathermy is set up with fine tipped forceps.
A Mixter and some sloops may be useful.
The limb is prepared up to the elbow and draped.

The patient is sent home with oral analgesia such as cocodamol.
The patient is instructed to elevate the limb.
A 1 week post operative appointment is made to check the wound and commence some hand therapy that includes nerve gliding excerises.
The sutures are absorbable and do not require formal removal.
The patient is reviewed at six weeks in the outpatient clinic.

There are no recent reported results of combined median and ulnar nerve decompressions at the wrist using the approach described.
Maroukis BL1, Ogawa T1, Rehim SA1, Chung KC2.
Guyon canal: the evolution of clinical anatomy.
J Hand Surg Am. 2015 Mar;40(3):560-5. doi: 10.1016/j.jhsa.2014.09.026. Epub 2014 Oct 29.
A historically relevant overview of the anatomy at Guyons canal
Kaiser R, Houstava L, Brzezny R, Haninec P.
The results of ulnar nerve decompression in Guyon’s canal syndrome. Acta Chir Orthop Traumatol Cech. 2012;79:243-8
About a third of cases in these series were associated with a ganglion. The vast majority improved significantly following decmpression.
Mondelli M1, Ginanneschi F, Rossi A.Neurosurgery.
Evidence of improvement in distal conduction of ulnar nerve sensory fibers after carpal tunnel release.2009 Oct;65(4):696-700.
Division of the transverse carpal ligament during a typical carpal tunnel release may decompress the ulnar sensory fibres as this neurophysiological study demonstrates.