This is a detailed step by step instruction through a Middle finger Proximal interphalangeal joint (PIPJ) cemented joint replacement with the Styker SR PIP joint implant via a dorsal ulnar approach.
This is a procedure usually performed for osteoarthritis of the PIPJ with stable collateral ligaments. It can also be performed for post-traumatic or well controlled inflammatory arthritis as long as the bone stock and soft tissue stability can support the joint.
The procedure can be performed as a day case under local, regional or general anaesthetic and take around 1 hour.
Following a period of 1 week in plaster cast the patient then starts mobilisation with a Bedford finger splint and is provided with a night resting splint at 30 degrees MCPJ flexion and straight PIPJs. The patient should achieve their pre-operative range of movement with minimal pain by 6 weeks and at this point should start strengthening exercises. The joint will always appear slightly swollen however the majority of post operative swelling will resolve by 3 months.

Indications
Articular damage causing pain in the PIPJ.
Failure of non-operative treatment.
Causes would include: osteoarthritis, inflammatory arthritis or post-traumatic arthritis.
Symptoms
The symptoms experienced are pain and stiffness which leads to reduced function and grip strength. In more severe cases night pain may be a problem for the patient. The operation is carried out in the main for pain. It will usually not improve the range of movement unless there is a specific bony block to the range. This is due to the progressive tightening of the soft tissues around the joint which remain in place and are repaired once the implants are inserted.
The patient’s job and hobbies often play a major role in their symptoms and therefore discussing these details and realistic expectations of the post-operative outcomes are essential in treatment selection especially if they have a very good grip strength despite the pain. Very heavy manual work is often a cause for the arthritis and exacerbation of the pain.
Examination
A patient with PIPJ arthritis who requires surgery will usually have a swelling around the joint which will be a combination of synovitis and osteophytes. The will often have a restricted range of movement in both flexion and extension and a reduced grip strength.
There is often some angulation at the joint due to an uneven collapse of the proximal phalanx condyles or erosion into the middle phalanx base. This is likely to be angulation in an ulnar direction due to the forces exerted on the joint by the thumb during tripod pinch in the index and middle fingers.
The joint may be painful to palpate and certainly be painful at extremes of movement. If they have considerable joint deformity and angulation (common in inflammatory arthritis) this would suggest poor soft tissue support and they would not usually be considered for this type of joint replacement. A single piece plastic joint replacement is usually more appropriate.
They may have other arthritc joints however it is not uncommon to have isolated PIPJ arthritis due to trauma.
Investigations
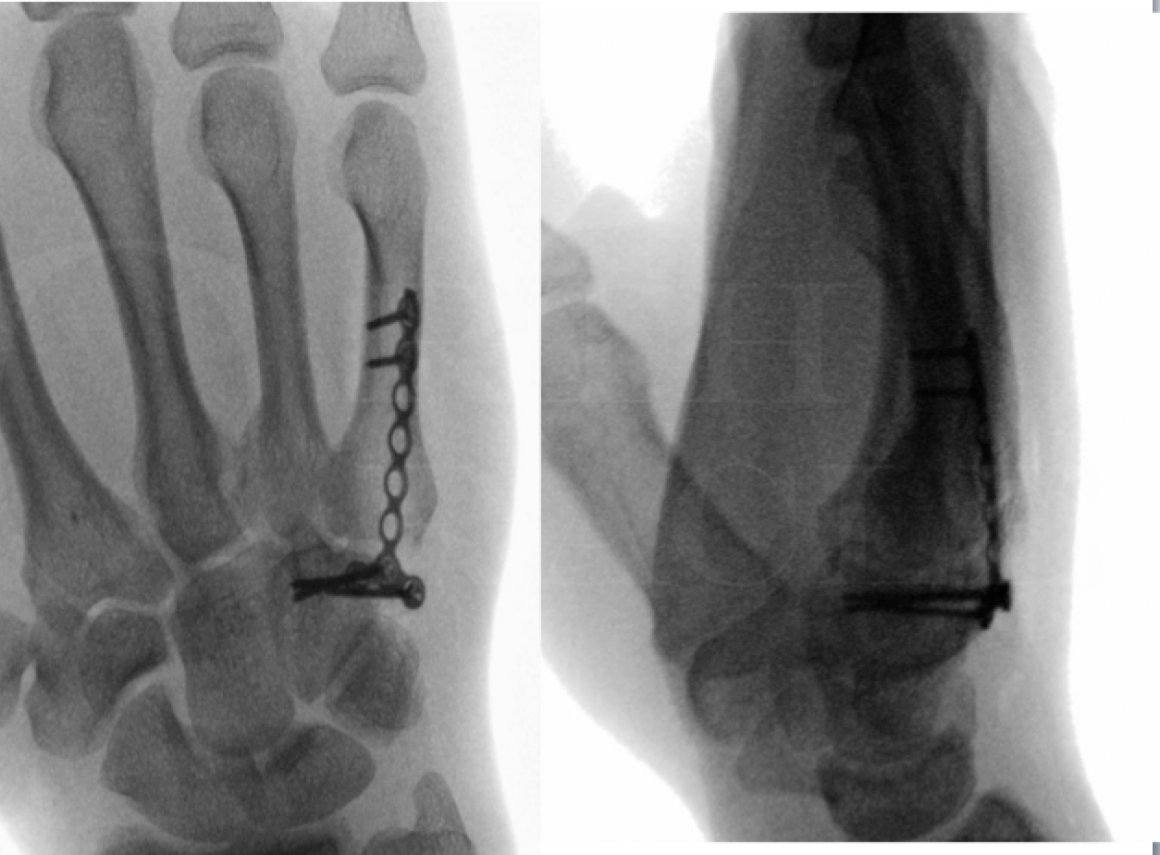
Investigations include plain PA and lateral radiographs of the effected joint.
Non-operative Management
Non-operative management for arthritis includes, analgesia, activity modification, Bedford splinting (which may be worn during certain activities and prevent accidental deviation and pain), physiotherapy with grip strengthening and steroid and local anaesthetic injections.
The injections treat the synovitis not the wear to the joint.
Alternative operative Management
Alternative procedures for PIPJ arthritis include:
Silastic single piece joint replacements, other bicomponent replacements.
Arthrodesis.
Denervation.
Contraindications
Absolute contra-indications
Infection, skeletal immaturity and joint instability.
Relative contra-indications
A very stiff joint which an arthrodesis may be a better option with fewer risks (particularly of revision surgery).
A heavy manual job – which is likely to cause early failure (often when patients are a couple of years from retirement it may be advisable for them to delay surgery until retirement to prolong the life of the implant).
A very distorted/collapsed joint – the soft tissues may be intact but very tight in this case and may require release to insert an implant- this group of patients may be best to be also consented for joint fusion or silastic single piece replacements with the option to convert inter-operatively if excessive soft tissue release required to insert a trial has made the joint unstable.

Pre-operative preparations and Equipment
The operation can be performed under local, regional or general anaesthetic. The duration of surgery is around 1 hour. An upper arm tourniquet is applied and inflated to 250mmHg (a digital tourniquet may also be used if performing the procedure under local anaesthetic and if it will not interfere with operative technique).
A clean air flow theatre is recommended for implant surgery and a change of gloves prior to implant insertion to reduce infection risk.
Equipment – Stryker SR PIP implant tray with range of implants XS-XL, narrow saw blade, Fine bone nibblers, bone cement, an image intensifier, plaster cast.
A single dose of antibiotics are given pre-operatively.

The procedure is performed as a day case and the patients are discharge with a sling and return within a week for wound review and hand therapy.
We provide paracetamol, ibuprofen, codeine and a laxative (senna) on discharge.
The wound is redressed and a Bedford splint applied to the finger. The Bedford splint is applied to the operated finger and its ulna neighbour to protect the elevated ulnar collateral ligaments. (taping may be required for a 5th PIPJ replacement to prevent excessive ulnar deviation as a Bedford splint will be a poor fit to its neighbour the ring finger).
At 2 weeks the dressing removed.
The Bedford splint is worn full time for 6 weeks and is used to prevent excessive radial or ulnar deviation and aid in mobilisation supported by the adjacent digit. A volar resting splint in 30 degrees MCPJ flexion and straight PIPJs is also provided for night time wear for 6 weeks.
At 6 weeks a PA and lateral radiograph of the joint is taken this is repeated at 6, 12 and 24 months.
Strengthening exercises can begin at 6 weeks and most patients should expect to have most of their grip strength and final range of movement by 3 months.
It will usually take patients 6-8 weeks to return to light work and 3-6 months to return to heavier work.

Results
Complications include infection, stiffness, continued pain, fracture and implant failure/loosening.
For some figures on these complications please read the following articles:
Thomas E. Trumble and Dennis J. Heaton. Outcomes of Surface Replacement Proximal Interphalangeal Joint Arthroplasty Through a Volar Approach: A Prospective Study. Hand (N Y). 2017 May; 12(3): 290–296.
This paper describes a series of 21 patients using the Stryker SR PIPJ as show in this operation but using a volar approach. There was a mean of 34 months follow up, a mean arc of motion at the PIPJ of 87 degrees which was an improvement from pre-operatively of 58 degrees. There were no implant failures, 4 (20%) extensor tenolysis and 1 superficial skin infection.
Murray PM1, Linscheid RL, Cooney WP 3rd, Baker V, Heckman MG. Long-term outcomes of proximal interphalangeal joint surface replacement arthroplasty. J Bone Joint Surg Am. 2012 Jun 20;94(12):1120-8.
This paper reviews the long term follow up of a similar metal on polyethylene 2 component prosthesis. 67 implants were followed up for a mean of 8.8 years. The majority were implanted for osteoarthritis via the dorsal approach and cemented in situ.
This paper reviews the long term follow up of a similar metal on polyethylene 2 component prosthesis. 67 implants were followed up for a mean of 8.8 years. The majority were implanted for osteoarthritis via the dorsal approach and cemented in situ.
At follow up the mean range of movement at the PIPJ was 40 degrees. Eight prostheses had failed. This equated to implant failure of 3% at one year, 8% at three years, 11% at five years, and 16% at fifteen through twenty-five years. Volar implanted joints failed more frequently than those inserted via a dorsal approach. The were no infections and overall 2 patients underwent amputation and 4 PIPJ fusions due to failures.